What is trauma?
Trauma is the lasting emotional response that often results from living through a distressing event. It arises from our nervous system’s attempt to process our overwhelm when we’re under distress.
In short, trauma is a response to a distressing event, not the event itself.
Trauma is like a wound. Although the wound may heal in time through adequate and intentional care, it will leave a scar. And if you push hard enough at the scar, it will still hurt. We need to respect our scars.
Unfortunately, many people do not get the chance to fully heal from a trauma wound before it becomes complicated and compounded by additional trauma wounds, like a scab being ripped off repeatedly.
We need to respect our trauma.
Types of trauma

- Single incident trauma — A response to a one-time sexual assault, a car crash, a terrorist attack, etc. Single incident trauma can often be healed in a few sessions with a certified Trauma Therapist who practices therapies such as Eye Movement Desensitization and Reprocessing (EMDR), Prolonged Exposure Therapy, Cognitive Processing Therapy (CPT), or Stress Inoculation Training. Trauma-informed talk therapy, such that we provide at CSAC, is also effective in helping unpack trauma.
- Complex/repetitive trauma — A response to repetitive sexual abuse, bullying, microaggressions, living in a war zone, etc. Complex trauma may take longer to process and heal from than single incident trauma. People with this repetitive trauma are sometimes diagnosed with Complex Posttraumatic Stress Disorder (C-PTSD).
- Developmental trauma — A response to adverse childhood experiences (ACEs), attachment wounds, etc. Developmental trauma occurs during our early development stages (infancy, childhood, adolescence) and can lead to mental disorders such as anxiety, depression, ADHD, etc.
- Intergenerational trauma — A response to inherited unhealed trauma from parents, grandparents, etc. Intergenerational trauma is hardwired from conception and is passed down through genetics and influenced by environment.
- Historical trauma — A response to the historical legacy of slavery, genocide, colonization, etc. Historical trauma is also hardwired from conception and shows up in people whose ancestors, culture, or community has been historically oppressed (e.g. African Nova Scotians, Indigenous peoples in Canada, etc.).
It is important to remember that trauma is treatable. Having a long-term, trauma-informed therapist is an effective way to talk through and receive emotional support for all types of trauma.
Trauma responses

Trauma responses can include anything from intense “fight, flight, or freeze” instincts, dissociation, and flashbacks, to more subtle coping strategies such as people-pleasing (fawning), emotional avoidance, and substance misuse.
The experience of trauma can harm a person’s sense of safety, sense of self, and ability to regulate emotions and navigate relationships. Long after a distressing event occurs, people with trauma often feel shame, helplessness, powerlessness, and intense fear. When thoughts and memories of the traumatic event don’t go away or keep getting worse, they may lead to Posttraumatic Stress Disorder (PTSD), which can seriously disrupt a person’s ability to regulate their emotions and maintain healthy relationships.
(Adapted from source: CAMH Canada)
Trauma and the brain
When our body’s nervous system becomes overwhelmed, it’s ability to process what’s happening gets “stuck.” This “stuckness” can result in physical, emotional, psychological, and behavioural responses such as nightmares, rumination, obsessions, flashbacks, emotional outbursts, dissociation, and being easily triggered by smells, sounds, movements, etc.
The following is an overview of how trauma affects different parts of the brain.
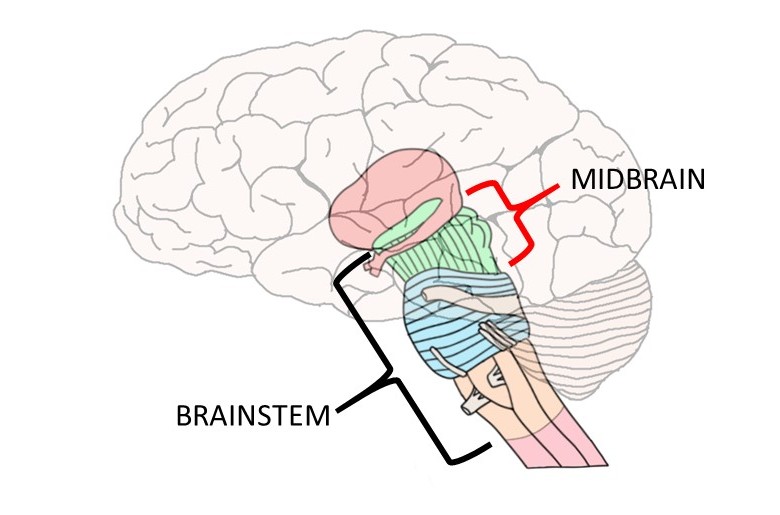
DOING BRAIN — Brainstem & midbrain
The brainstem and midbrain are responsible for survival-related functions including controlling heart rate, breathing, body temperature, eating, sleeping, and pain. They also store anxiety and arousal traits resulting from traumatic experiences.
Unresolved trauma keeps the sympathetic nervous system activated and prevents the parasympathetic nervous system from kicking in, which keeps the body in a state of hyperarousal. When we’re in this hyperaroused state, blood leaves our brain in order to engage our extremities and, in doing so, causes us to become anxious, easily triggered, hypervigilant (e.g. easily startled), unable to achieve REM sleep, etc.
This is why an important part of trauma work is helping to reactivate the parasympathetic nervous system. Therapeutic techniques such as mindfulness, deep breathing, meditation, yoga, and progressive muscle relaxation can help put our bodies in a calm state to process trauma.
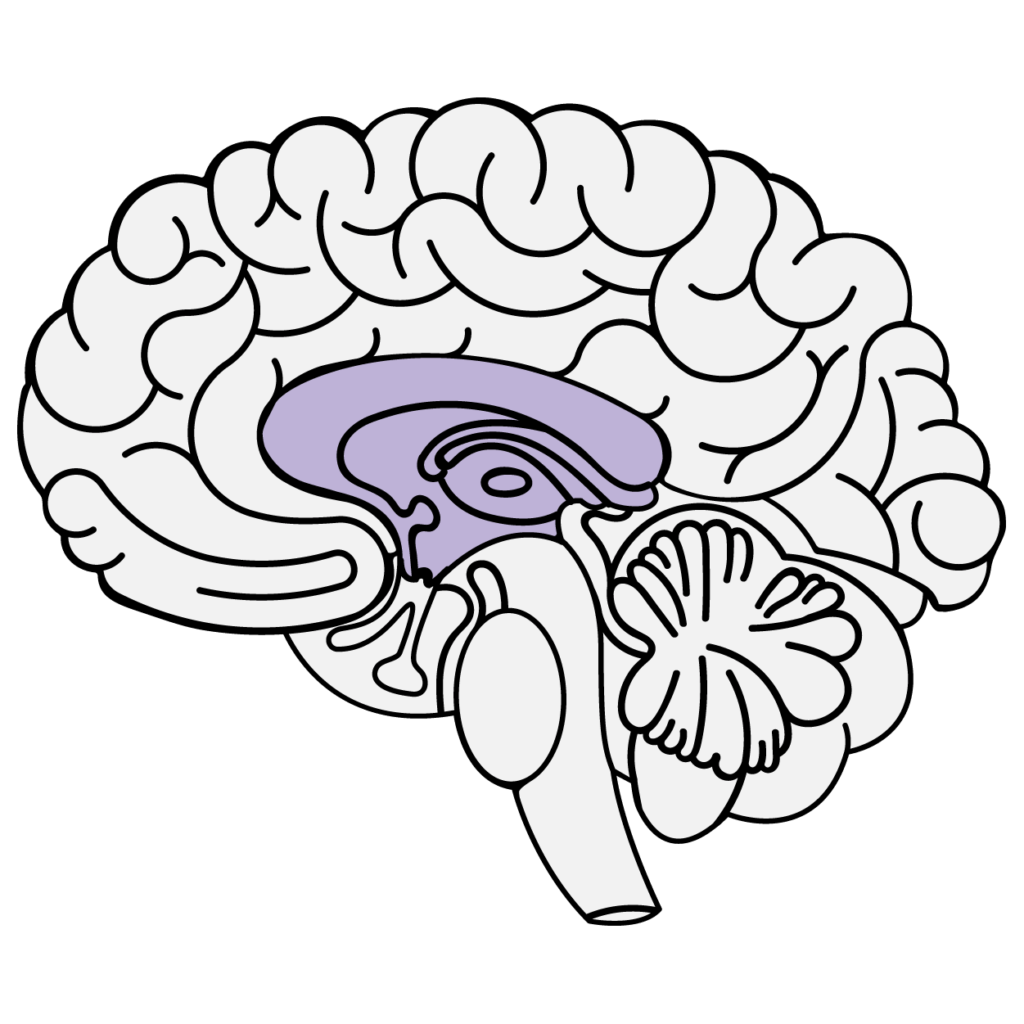
FEELING BRAIN — Limbic system
The limbic system is the emotional centre of the brain, made up of the hippocampus, amygdala, and anterior cingulate gyrus. The hippocampus is largely responsible for turning short-term memories into long-term memories and the amygdala takes care of processing our emotions.
In trauma, the amygdala is flooded and in an intense emotional state, which prevents the hippocampus from processing trauma in the left (logical) side of our brain where memories normally get encoded with language. This is why it is often difficult to “speak” or “voice” trauma in words: our brain simply wasn’t able to connect the traumatic experience (sounds, smells, feelings, etc.) to language at the time the event took place. Without language, our trauma memory becomes “stuck” in our brain with no way to escape.
Because memory is largely stored in the right (intuitive) side of our brain, trauma work that involves creativity and imagination helps to process the trauma that is stuck without language. Therapist-facilitated techniques such as creating art, working with clay, sand tray activities, and instrumental music can help to process trauma.
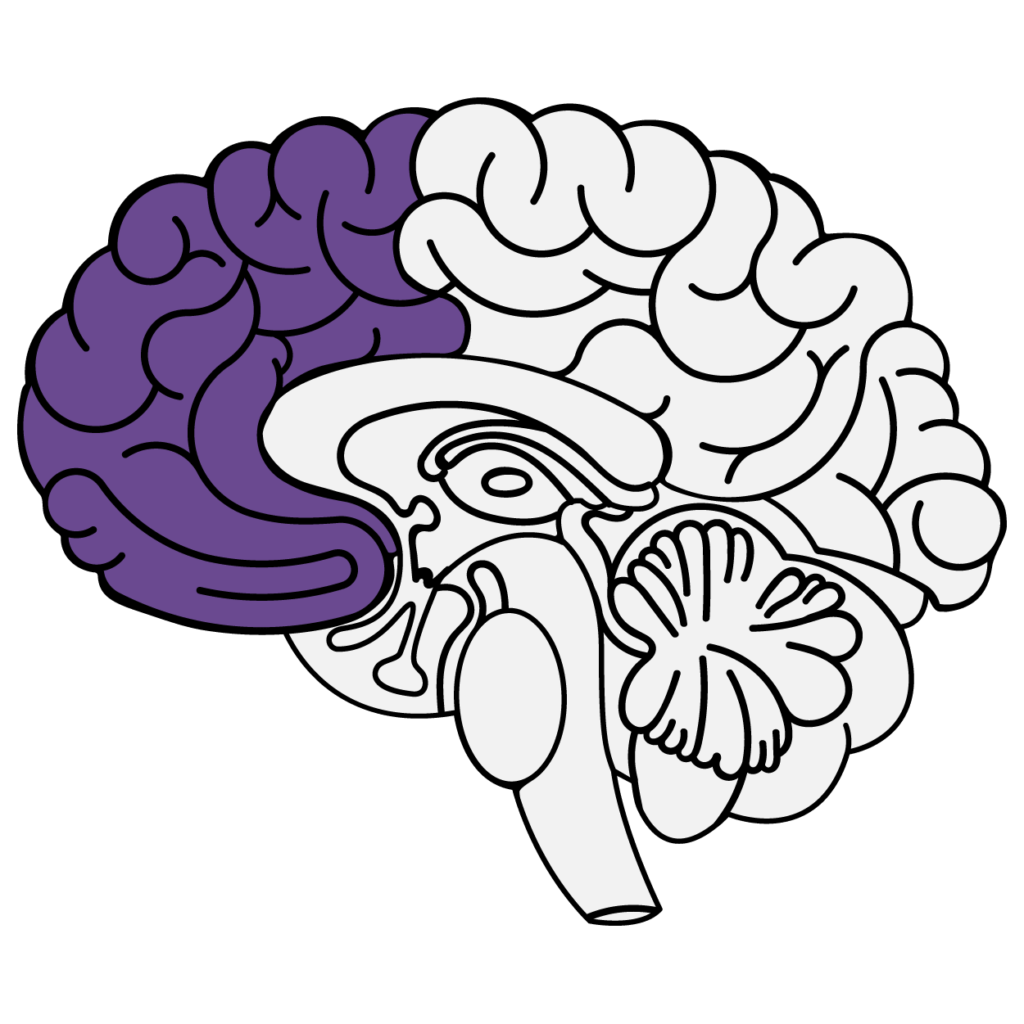
THINKING BRAIN — Prefrontal cortex
The prefrontal cortex is responsible for executive functions (focusing, following directions, etc.), thinking, perceiving, reasoning, logic, planning, problem-solving, making good decisions, and regulating emotions.
In trauma, a phenomenon called hemispheric dissociation occurs, which prevents the two sides of the brain from communicating due to overwhelm. This fundamentally alters the structure and function of the brain, which can lead to mental disorders such as Generalized Anxiety Disorder (GAD), Major Depressive Disorder (MDD), Posttraumatic Stress Disorder (PTSD), Attention Deficit and Hyperactivity Disorder (ADHD), Dissociative Identity Disorder (DID), Borderline Personality Disorder (BPD), etc.
However, just as trauma can cause damaging structural changes in the brain, trauma therapy can also restructure the brain back to its healthy, full-functioning self. The ability of the brain to heal is called neuroplasticity. Many types of trauma therapy (EMDR, Exposure-based, Art & Play based, etc.) have been scientifically proven to help change the structure of the brain. Trauma-informed talk therapy is also useful in helping unpack, understand, and cope with trauma.
Trauma is treatable. There is hope.
External Resources:
Trauma & The Brain — A comprehensive overview by the Younique Foundation of how trauma affects the brain, including healing resources.
Trauma Big and Small: Why It All Matters and How to Cope — An article outlining the difference between ‘big T’ and ‘small T’ trauma and the impacts.
The Freeze Response and Sexual Assault [YouTube video] — Many people have heard of the “fight or flight response” but fewer have heard of the “freeze response.” The freeze response is your brain’s most desperate attempt to survive in the face of an overwhelming or overpowering danger. Many people impacted by sexual assault and harassment freeze in the moment, or they automatically comply, smile or appease their abuser, then later feel ashamed for doing it. This video explains why that freeze response serves an ancient survival function, and also some potential options for how to turn off the freeze reaction and respond in more intentional or helpful ways when one’s life is not at stake.

